How to Engage with a Patient and their Family during a Telehealth Visit?



How can we make sure telehealth processes are making a difference that matters? Having led virtual care for Kaiser Permanente Colorado, what matters most to me is that we are finding ways to make care less expensive and/or with better clinical outcomes.
We have some proof that telehealth improves clinical outcomes. Video visits significantly decrease no-shows for mental health care. Remote patient monitoring significantly increases patient engagement in managing chronic disease. Most trust that no-shows and patient engagement are good surrogates for improved outcomes. However, the evidence that telehealth processes lead to decreased cost and/or improved clinical outcomes is less clear.


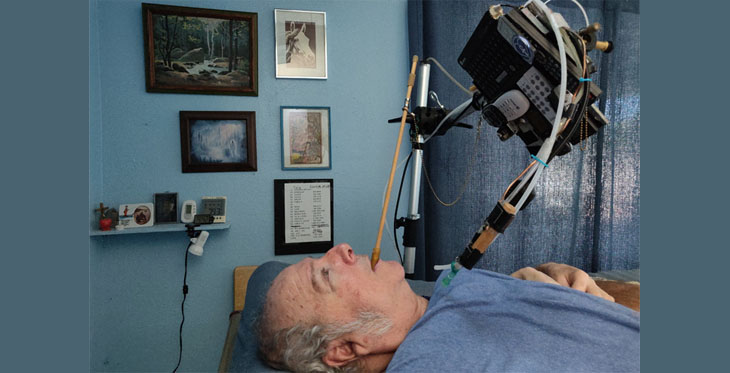
I don’t use a smartphone to access Telehealth. Being a “tetraplegic” I have no use of my hands, so I invented a unique way to operate different electronic devices.
I created two styles of mouth sticks.
This one I use while in bed. It’s made from a quarter inch wooden dowel with both ends covered with surgical tubing. If you notice, one end is covered two and a half inches and the other a half inch. The longer end is for biting on and the other is to cushion the tip.
The second mouth stick I use while sitting up in my wheelchair. I can drive up to the desk I designed and park myself in front of my keyboard and computer. The mouth sticks I use while in my chair has a lucite bite impression the dentists made for me. I don’t use this type of mouth stick while laying down in bed because I can’t easily swivel the stick from side to side.
I’m not ready to jump on a plane anytime soon to get away from staying at home during COVID, but I am willing to jump in my car and take a road trip to do some hiking in National Parks on less popular trails and have done just that in the past couple of months. One was to Great Smokey Mountain National Park and the other to Shenandoah National Park and the Blue Ridge Parkway.



