In May, the Navajo Nation surpassed New York and New Jersey for the highest per-capita infection rate of COVID-19 in the US.
In an area where 30 to 40 percent of residents don’t have running water and families live together in multigenerational homes, containing the spread has been difficult. In addition, residents can’t stay at home and see a healthcare provider using telemedicine, as so many of us have been able to do during the Public Health Emergency, because there’s little to no cell service or internet availability. So anyone needing healthcare or showing symptoms of COVID-19 has to travel to one of the few healthcare facilities.
At the Indian Health Service (IHS) site Chinle Comprehensive Health Care Facility in the center of the Navajo Nation, staff got very innovative very fast to provide healthcare services while keeping patients and providers as safe as possible.
Stephen Neal, PA-C, is the Chief of Staff at Chinle and also works in Informatics and Family Practice. He says that—luckily—they had already been working on developing Chinle’s first telehealth program, for rheumatology, before the pandemic began. He had already obtained the equipment: four videoconferencing displays and ten video phones. “We’re lucky to have them,” he says, “because they’re now on back order.”
Chinle staff needed to decide how and where to deploy the telehealth equipment and how to save their limited PPE and protect their workforce. Numerous staff had been quarantined during the pandemic, especially at the start, so it was imperative to keep them healthy and able to work.
IHS had a functional telemedicine platform with limited deployment, and requested Chinle to be a test site to evaluate rapid enterprise deployment. To test as much as possible, Neal opened it up to the entire medical staff—optometry, occupational therapy, women’s health, physical therapy, pediatrics, etc.—and taught them how to do telemedicine visits. Unfortunately, due to the lack of appropriate (or in most cases, any) bandwidth availability, telehealth couldn’t work successfully in the field. However, it has worked out beautifully at the facility.
- For COVID-19 screening, providers use the equipment to see patients who are in a separate room 30 feet away. Patients go into the room and sit on a chair, which is the only thing they touch; the telehealth equipment automatically turns on. Providers are not exposed to patients directly, so it saves PPE and prevents provider exposure. Chinle has had about 4,500 visits in this screening /respiratory clinic since March—and now, thanks to this system, they haven’t had a provider quarantined in 10 weeks.
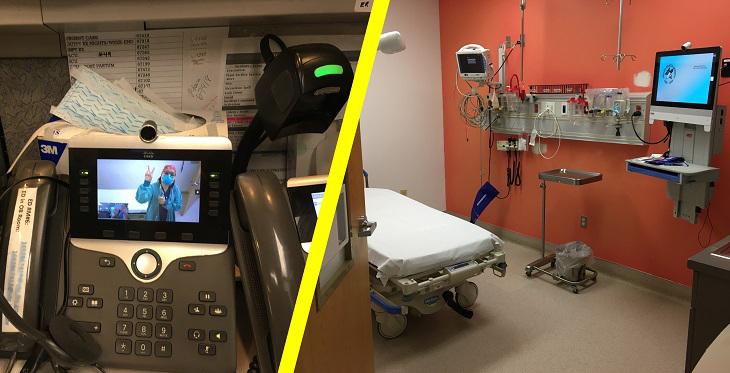
- In the ER, providers were getting slammed with COVID-19 cases, and the visibility into the negative pressure rooms was limited, so staff set up video endpoints in the negative pressure rooms. Now nurses can easily monitor and talk to the patient without having to don PPE—and someone at the nurses’ desk can do charting while a provider is in with the patient.
- Pediatric and adult care units were partly converted to respiratory care units. Because Chinle has had a high COVID-19 burden, those rooms are constantly in use and, thanks to the telemedicine equipment, outside staff can observe and document during intubation without having to don PPE.
- In the inpatient unit, rooms originally had a speakerphone and a lot of providers crowded into the room. This didn’t work well, so staff swapped out the phone for a video phone. This is keeping providers from having to don PPE and helps immensely with observation and documentation for high-risk procedures. “It comes down to, ‘we have a problem; could telehealth solve it?’” says Neal.
- All the nephrology clinics have been converted to telemedicine for about nine weeks now. Patients come to the Chinle clinic because their homes don’t have broadband access; the nephrologist beams in from a remote location or even on site in a separate room.
- Telemedicine has been useful in easing patients’ concern about potential exposure to COVID-19 from providers. “They would way rather talk to them through a machine at a safe distance,” Neal says.
Chinle staff also have come up with innovative ways to use the technology to, ironically, bring people closer. Neal cites the case of a mom who delivered a baby and found out she was COVID-positive. She was in isolation with her baby and very upset, so staff installed a video endpoint in her room. “She was so happy to be able to see people and be engaged and not isolated,” he says.
And the technology is helping staff as well. It’s been a very tough time for providers, and they use the secure platform for provider support groups.
Neal says they were initially worried about patient acceptance of telemedicine, especially among elderly patients. However, they haven’t had a single issue. “Patients have all not only accepted it, but felt much better with it because they don’t want to be exposed to the providers,” he says. “It protects them.”
There’s been plenty of innovation outside of telehealth at Chinle too—for example, buying Gore-Tex and Tyvek and having a sewing committee make washable, reusable, disinfectable gowns; using Microsoft OneNote to share information like EHR processes, scheduling, and triage flow charts among providers; and creating a PPE matrix showing capacity and need for rationing.
Chinle is also looking at more telehealth innovation and is about to pilot a new program. “We want to send tablets into patient homes,” Neal says. The tablets can use the FirstNet network, which is set up for first responders. Chinle has a group called Baa Hózhó, which translates to “Better Care, Lower Costs.” Community Health Representatives will go to a patient’s door, give them the tablet, and have them meet with whatever providers they need to see—including podiatrist, medical provider, diabetes educator, and dietician.
It’s been an explosion of telehealth deployment for Chinle and IHS at large, Neal says. And most importantly, it has helped to keep patients and providers safe.
(Photo: Chinle Service Unit ED using telemedicine tools for poorly visible negative pressure rooms. Photos courtesy of Stephen Neal.)


