
No – not that first time! How was your very first telemedicine visit? Since the beginning of the COVID pandemic back in March a significant number of people have had their very first telemedicine visit. Surprisingly, even though I’ve been involved in telehealth for over 30 years, I actually fall into that group of “newbies”. I am very fortunate (knock on wood) to be overall quite healthy. My typical medical routine consists on an annual physical, annual mammogram and dental check-ups every 6 months for the most part. Breaking my leg skiing in 2019 – trust me – that surgery could not have been done remotely and the rehab really required all the cool tools and devices my physical therapist had on site.
So why did I need a telemedicine visit? I love working in the yard. When I lived in Tucson this meant cactus prickles, mesquite thorns and bumps, bruises and scrapes from trying to dig through caliche to install or fix irrigation to water the few plants that would actually grow in the desert. Although there are nasty bugs and critters of all sorts, the worst I ever had was a scorpion bite on my finger – and that happened while I was sleeping! With no other symptoms than pain and numbness, with a little online research that got solved with ice and time. Moving to Atlanta brought trees, flowers, grass – a real East coast yard! Lots of outside work for me to do on weekends but also new things to watch out for. There’s actually a lot of the same bugs and critters – snakes (yes poisonous ones too), black widow and other spiders, coyotes, ants (fire in particular), no Africanized bees (yet) but we have bees, wasps and yellow jackets (and I don’t mean GA Tech), and with all these trees ticks and chiggers. Add in poison ivy, poison oak, Virginia creeper and other very pretty but potentially irritating plants and you have a lot to look out for when working outside.
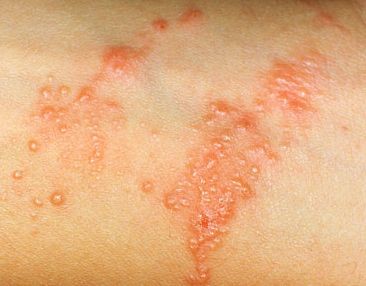
Needless to say, a few weeks ago I touched or got touched by one of these sneaky little plants or bugs and developed a rash. It’s happened before (yes I wear long sleeves, pants, hat, gloves and use bug spray but the plants and bugs really are sneaky) so I started out self-treating for contact derm – the ever-popular pink calamine lotion and Benadryl. That helped a little but the rash continued to spread so after a week I decided it was time to call my dermatologist. When I called they asked whether I wanted an in-person or telemedicine visit – I chose telemedicine and had an appointment for 2 hours later. The scheduler took my email address and sent me a link (FaceTime) for the visit. She explained that I would see the nurse first to go over some things and then the dermatologist.
I took a few still images of the key rash locations with my cell phone (using the lighting, angle, distance and background tips I knew from working on the American Telemedicine Association’s Teledermatology Practice Guidelines) and quickly uploaded them to the portal. They didn’t ask for them but I figured it would likely be easier and clearer than with my iPad camera live and in any case would give the dermatologist a preview. At the appointed time, I logged in and there were the two nurses (in the office). They explained the telemedicine visit process and made sure I understood what would happen, verified my consent to engage in telemedicine and then I explained my problem to them and noted that I had uploaded some pictures. They took notes (obviously on their iPad which must have been connected to their electronic health record) then said it was time to switch over to the dermatologist. First try it didn’t work – seems FaceTime has an issue bringing in a third party sometimes. They re-connected and said he would just have to connect directly so we hung up and then he connected. This took 2 minutes max to solve the connection problems.
My dermatologist was clearly at his house (hats off to the nurses who were at the office!) and he had done a good job of having a non-cluttered room and background, good camera, good lighting and good audio. I summarized the problem, held up my arm that had a rash patch, he had already looked at the images I sent and said – yup it’s contact derm and I’d been doing all the right things but a stronger cream and a course of Prednisone would do the trick. He wrote and submitted the prescription to my pharmacy and handed me back to the nurses. They made sure I understood what he had prescribed and what I was supposed to do. By 10:20 I was seen, diagnosed and had my treatment – happy as a clam! The billing person called about 30 minutes later for my co-pay and later that afternoon my prescription was ready to pick up. I was one very happy telemedicine patient!
Having this experience, I asked the rest of the Arizona Telemedicine program team if they or any of their family members had any first time stories they would like to share.
According to Mary Weinstein (ATP Director Ron Weinstein, MD’s wife), “I met my new Internist last Wednesday for the first time in a 45 minute video Telehealth visit. It was initially supposed to be an office visit but our hospital system is currently doing all well-patient office visits as either audio only or video sessions. I was a little apprehensive about having our first meeting not be in person but was delighted to realize that within five minutes I was completely comfortable and fully engaged. The 45 minutes flew by and I signed off feeling very connected to my doctor and delighted that it had been such a positive experience!”
Kris Stewart’s niece Payton Stauch recalled, however, that, “Back in March I had a telemedicine visit with my PCP. I was excited about trying this new medium of interaction. It seemed so ideal to be able to see my doctor from the comfort of my living room. Unfortunately, the connection was terrible and we could barely hear what the other person was saying. She mentioned her telehealth visits tend to cooperate more in the mornings and my visit was in the late afternoon. Although I think telemedicine is an amazing technology that will be highly utilized in the near future I will be sticking to in person visits with my doctor whenever possible for the time being.”
It was interesting to hear the contrast in the three experiences and I’m sure that reflects the status of telemedicine overall. Even though COVID has led to much wider and rapid adoption of telemedicine, it is clear that there is still quite a lot of work that needs to be done in a variety of areas to optimize the experience under all possible circumstances, conditions, clinical specialties and practice/institution types. Stories like these are becoming much more common (hopefully more on the positive side) and for those of us who have been and are engaged in trying to make telemedicine more mainstream, they may just represent the push that’s needed to really get us there.


