How Does a Telemedicine Pain Program Work in Rural America with Multi-Vulnerable Patient Populations?

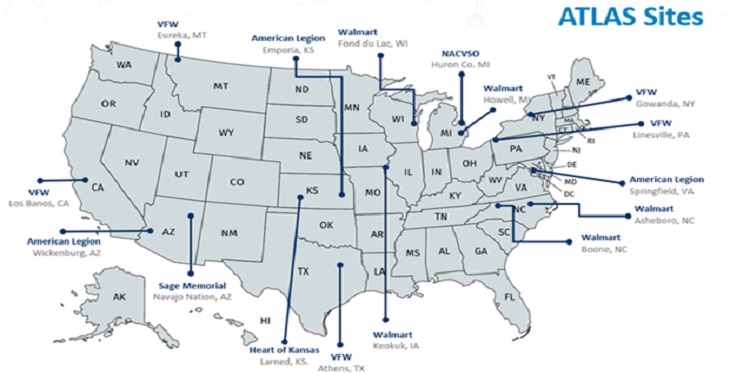
In April 2017 Summit Healthcare started a multi-disciplinary program to treat patients with chronic and acute pain in the White Mountains of Arizona. Our patient service area is HRSA-designated as having a shortage of providers and medically underserved. The area is the size of Rhode Island and includes Native American reservations and other vulnerable populations. Many of our patients live in a high poverty area which makes access to care challenging.